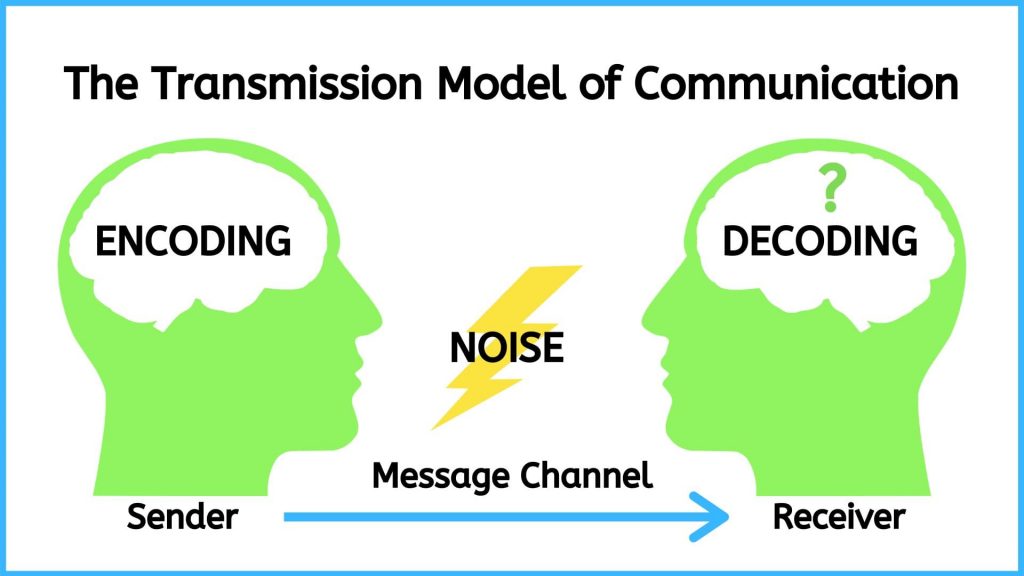
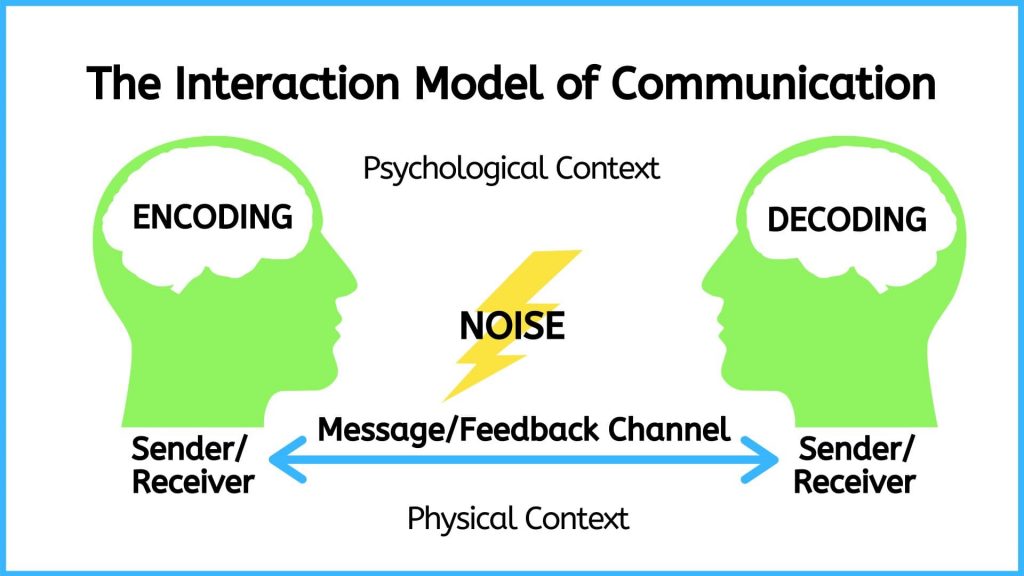
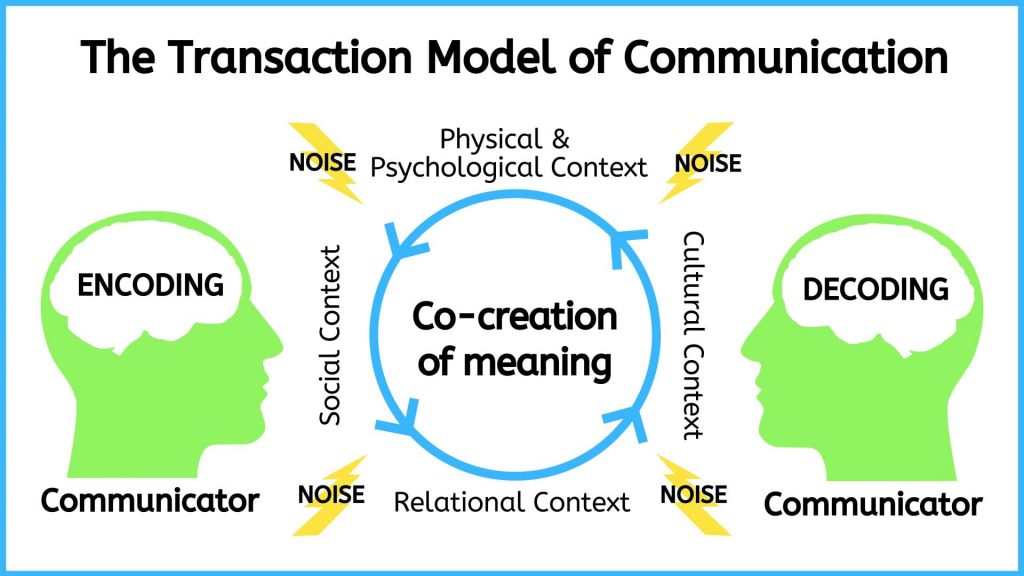
Relational inquiry is defined as “the complex interplay of human life, the world, and nursing practice”. This means that nurses must avoid looking at the client on a merely individual level. As per Doane and Varcoe, drawing upon relational inquiry involves the following elements of communication:
- Intrapersonal – communicating with the client in a way that allows you to assess what is occurring within all people involved (the client, you, and others).
- Interpersonal – communicating with the client in a way that allows you to assess what is occurring among and between all people involved.
- Contextual – communicating with the client in a way that allows you to assess what is occurring around the people and situation involved.
Relational inquiry is a kind of lens you can use to perceive the world. In contrast to an individualist approach, which privileges the individual as accountable for their actions and behaviours, relational inquiry brings into focus the internal dialogue of the client, their social system, and the broader context that influences their actions and your actions as a nurse. This approach to therapeutic communication is important because it can help you understand the client’s situation more fully, focus on what is important to them, and collaboratively work with the client to integrate this knowledge into the care.
See Case Study 2 for an example of a relational inquiry approach to interviewing.
Case Study 2
An 8-year-old client, who uses the pronouns he/him, attends a pre-operative day surgery unit for tonsillectomy (tonsil removal) with a parent present. The client has a history of 6 strep throat infections with antibiotic treatment in the last 18 months. The client has no previous history of surgery or anaesthesia.
RN: Hello Peter Lin, my name is Ahsan Khan, I am a registered nurse. I will be caring for you until you go into surgery and then a surgical nurse will take over your care. You can call me Ahsan. What name would you like me to call you?
Client: Peter.
Rationale: You introduce yourself using first and last name and explain designation – this action promotes accountability. You explain the extent of the care being provided, including when it will end and who will take over care for the client at different stages of their procedure. This includes the client in the care plan and minimizes uncertainty about care provision.
RN: Okay, Peter. The information you share with me will only be shared with the healthcare team involved in caring for you. Before we begin, who is with you today?
Client: It’s my mom.
Rationale: You explain confidentiality at a developmentally appropriate level for an 8-year-old. Asking the client “who is with you today” allows the client to identify their relationship to their caregiver in their own words.
RN: [directed to mother] Hello, what would you me to call you?
Client’s mother: Please call me Wei.
Rationale: This approach includes the mother in the care and acknowledges her participation. Some providers refer to the parent as mom or dad as this reinforces the client (child) as the recipient of care and is also convenient for the provider for easy reference. However, calling the parent by their preferred name builds trust and rapport, acknowledges their humanity, and identifies them in the care process.
RN: Okay, Wei. [directed to both client and client’s mother] I will collect some information from you and then do a physical exam. It should take about 10 minutes. I can see in your chart here that you are scheduled for a tonsil removal and that you have signed a consent form. Can I answer any questions you have before we proceed?
Rationale: Repeating the preferred name of the client’s mother helps you remember the name, while also acknowledging the mother’s request. You offer the client and mother a timeline and plan to help them anticipate events. You invite any questions before conducting the subjective data collection. This can be a helpful tool for you to gauge the client and can also alleviate concerns up front.
Client and Client’s mother: Not really.
RN: Ok. Can you tell me about how you are feeling today, Peter?
Rationale: This question invites an intrapersonal response as it attends to feelings and emotions for the client. Most importantly, it acknowledges the importance of his thoughts and emotions as part of their care (rather than ignoring them) and gives you the opportunity to respond to any concerns.
Client: A little nervous. Will I be able to feel anything during surgery?
RN: No, you won’t feel anything during surgery. We will give you some medicine to put you into a deep sleep and when you wake up it will be over. We will also be giving you some medication for pain.
Rationale: Your response attends to the client’s concern directly by providing a definitive answer. In this case, you also anticipate the client’s concern for pain as the concept may not be well understood, given the developmental stage.
RN: How are you feeling, Wei?
Client’s mother: I’m little nervous to give Peter pain medications.
Rationale: The question invites the mother to share intrapersonal concerns about the client’s surgery. This conveys to the mother a family-centred approach, whereby they are also a care recipient.
RN: Tell me more about your concern.
Client’s mother: Well, you read so much nowadays about opioids and addiction problems caused by prescribed medications. I’m worried about Peter.
Rationale: This approach invites discussion without supposition.
RN: I can understand your concern. The pain medications the anaesthesiologist administers during the surgery are short-acting, only a couple of hours. The anaesthesiologist will speak with you just before the surgery and you can ask more specific questions at that time. After the surgery is over, the surgical nurse will make sure Peter is comfortable and will likely give him medication for pain and swelling. You can continue this treatment when you are home with Peter. Both acetaminophen and ibuprofen are over-the-counter medications and not opioids, nor are they addictive. The surgical nurse will give you specific instructions about discharge care as well as a handout. If you don’t get this information, feel free to ask.
Rationale: In this case you respond directly to the mother’s concern about pain medication while anticipating the plan of care and other points of interface with the healthcare system. This offers reassurance about future opportunities to ask and clarify concerns. Importantly, in addition to letting the mother know what to expect, you also invite the mother to ask questions. This validates the mother’s concern and also alleviates others in the event they do not provide information.
Client’s mother: Ok, that’s reassuring. I have two kids home sick from school today with the flu. Will that be an issue for Peter?
RN: It could be. Hand-washing and keeping some space from each other if possible, will be important to minimize the spread of germs. Peter will be more susceptible to getting sick after surgery.
Rationale: This explanation responds directly to the mother’s question and offers strategies to reduce the risk of spread of germs. The response is also in everyday language, free from professional jargon.
Client’s mother: Oh boy, I’ll try.
RN: Tell me about your support system to help you manage at home.
Client’s mother: I have a good support system. My sister is really helpful with the kids, and she’s in town to give us a hand.
Rationale: In the context of this case scenario, this question assesses interpersonal relations by asking about support systems for managing this situation.
RN: That sounds like a helpful support. Are there other resources that would be helpful to you?
Rationale: This question helps assess the contextual relations through the identification of resources, and contextual issues that may require attention in this scenario. It invites further discussion about factors to consider in Peter’s care and sheds light on context for the dyad.
Client’s mother: Well the thing is that this has all come at a difficult time. I’m transitioning jobs, so money is tight right now. I don’t have extra room in the budget for a sitter. I’m glad my sister is coming, I just don’t know how long she can stay. I guess my parents could help in a pinch, but they are getting older and the kids are a lot for them to manage. And poor Peter has been sick so much lately. On one hand, I’m glad Peter will be getting the surgery to prevent other cases of strep throat, but I also feel badly that this is happening at such a stressful time for everyone. And I’m worried about the recovery time.
RN: I can see how that would be stressful. It’s going to take a few days for Peter to recover. The important thing will be to avoid the spread of germs as that could extend his recovery time. And you’re right that this surgery should help reduce his risk for getting strep throat in the future. It sounds like you have some alternative ideas for support to help you manage the recovery.
Rationale: This response offers empathy and encouragement by acknowledging what the client’s mother has shared and their support system. It also offers strategies to minimize recovery, which seems to be a concern identified by the mother.
Client’s mother: I do. Thanks.
Summary
A relational care approach attends to the broader social context in which clients and their support systems are situated. Also, as the nurse, you should be aware of yourself and how you influence, and are integrally connected to, the client and the healthcare system. This approach is an especially helpful tool for family-centred care. It also requires skill and knowledge because it demands active listening and critical thinking. Unlike closed-ended checklists, you cannot predict how the conversation will unfold.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.nscc.ca/healthcommunication/?p=46#h5p-8
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.nscc.ca/healthcommunication/?p=46#h5p-9